Disease Outbreak Map Flags 3% of Earth as Highly Vulnerable in New Global Warning
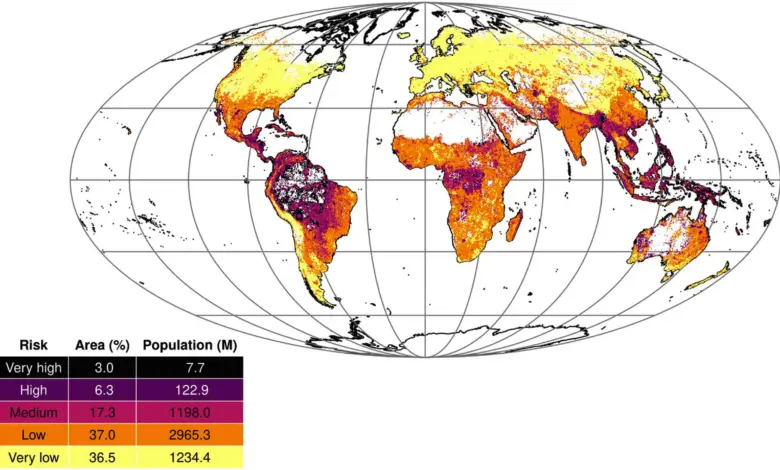
A new disease outbreak map is drawing attention for what it leaves little room to ignore: risk is no longer evenly spread. Global modeling suggests that 6. 3 percent of the world’s land area falls into a high-risk category, while another 3 percent is classified as very high risk. The concern is not just geography, but timing. As climate pressure intensifies and land development advances, the same places most exposed to ecological change are also the least prepared for the next spillover event.
Why the new map matters now
The study maps epidemic-prone diseases across nearly every country on Earth using machine learning and satellite data. Its central finding is stark: about 9. 3 percent of the world’s land area is highly vulnerable to dangerous outbreaks, with hotspots concentrated in Latin America and Oceania. That concentration matters because these regions are already under strain from climate change and land development, which can compound exposure rather than simply add to it. In that sense, the disease outbreak map is less a static chart than a warning about converging pressures.
The human toll is not captured by land area alone. The model indicates that roughly 20 percent of people live in medium-risk areas, while 3 percent inhabit zones of high or very high risk. That gap suggests a world where many communities are not in the most dangerous zones, yet still live close enough to face changing threat patterns. The practical challenge is not only where outbreaks may occur, but whether health systems can detect and contain them quickly enough.
What the science says about spillover risk
The research was led by Angela Fanelli, a veterinary epidemiologist at the European Commission’s Joint Research Centre. Her work focuses on how human-driven environmental change shapes epidemic risk and strains countries’ ability to respond effectively to crises. That framing is important because it links outbreak risk to the way land, water, and settlement patterns are changing over time. The disease outbreak map reflects that broader shift rather than a single pathogen or one isolated event.
Most of the diseases highlighted in the map are zoonotic, meaning they move from animals to people through infection and contact. One overview estimated that around three quarters of emerging infections in humans worldwide start in other animals. The mechanism is familiar: when people expand settlements into forests or wildlife markets, crowding raises spillover, the moment when a virus crosses into humans. The map also shows that all of the World Health Organization priority diseases included sit on a short list of carefully monitored dangerous zoonotic threats.
Climate stress deepens the problem. The modeling suggests that higher temperatures, heavier rainfall, and deeper droughts all push outbreak risk upward. Recent research also links climate change with altered migration routes, breeding cycles, and habitats that bring wildlife closer to people. Longer warm seasons allow disease-carrying mosquitoes and ticks to survive in new places, which can push previously tropical infections into higher latitudes. In other words, the geography of disease is no longer fixed.
Environmental pressure and public health vulnerability
Land use is the other major force shaping the map. Clearing forests for farms, roads, and mines moves people into closer contact with wildlife that can carry new viruses and pathogens. Dense settlements and industrial farms then create conditions where viruses can jump and spread more quickly. That interaction between development and exposure is one of the clearest findings in the disease outbreak map: environmental change does not just alter landscapes, it alters the odds of transmission.
The implication is that outbreak preparedness cannot focus only on hospitals and laboratories. It also has to account for where people live, how land is used, and how climate change is redrawing the boundaries between humans and wildlife. The map’s regional pattern, especially in Latin America and Oceania, suggests that vulnerability is highest where multiple pressures overlap rather than where one factor dominates.
Regional and global consequences
For governments and health agencies, the model offers a useful but unsettling message. Countries that are least equipped to detect and contain outbreaks may also be among those facing the greatest environmental exposure. That mismatch can turn an early warning into a delayed response, and a delayed response into a wider crisis. The disease outbreak map therefore has consequences that extend beyond epidemiology: it speaks to planning, land management, and climate adaptation.
It also raises a broader question about global resilience. If dangerous outbreaks are becoming more likely where ecological disruption is greatest, then prevention may depend as much on environmental policy as on medical readiness. The central issue now is whether institutions can act on that insight before the next spillover moves from risk model to real event.





