Caltech’s Whole-Body Ultrasound Breakthrough Exposes the Limits of Traditional Imaging
In a field where handheld probes still dominate routine care, caltech researchers have now demonstrated a system that can image an entire human cross-section instead of only a partial slice. The significance is not just technical. The work suggests that some of the most familiar limits in ultrasound are not inherent to sound itself, but to the way the technology has been used.
What did Caltech actually build?
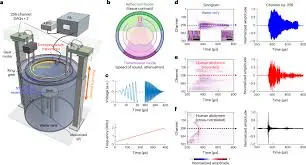
Verified fact: Lihong Wang, Bren Professor of Medical Engineering and Electrical Engineering, and a team at Caltech developed a whole cross-section ultrasound tomography system, or UST, designed to image humans in both reflection and transmission modes. The system uses a custom 512-element circular ultrasound receiver array and a rotating transmitter. In tests on five healthy volunteers, the team scanned the abdomen for 10 seconds at a time and produced two-dimensional images of the entire in vivo cross-section.
Verified fact: The images showed strong agreement with clinical magnetic resonance imaging counterparts. The system also produced images of the thighs, and the reported resolution was uniform in-plane across the cross-section. That matters because conventional ultrasound is constrained by a limited field of view, operator dependency, contact-induced distortion, and a lack of transmission contrast.
Analysis: The immediate implication is that ultrasound may be able to move beyond a narrow, probe-bound view of anatomy. The Caltech result does not replace existing imaging, but it does challenge the assumption that ultrasound must remain partial, local, and highly dependent on who is holding the transducer.
Why does the keyword matter to the clinical problem?
Traditional ultrasound works by sending high-frequency sound into the body and measuring echoes. In this system, water plays a central role because ultrasound propagates more efficiently through water than air. Wang explained that participants sat in an immersion tank with their heads out of the water, while a lab-made ring structure around the tank used 512 transducers to scan up and down the body. That arrangement allowed imaging of different cross-sections without compressing tissue.
Verified fact: The team also measured transmission signals, not only echoes. That allowed them to quantify the speed of sound and the attenuation of each wave as it was absorbed or deflected in the body. Wang said that when tissue varies, those measurements can help distinguish tissue types and may be useful in disease contexts such as chronic inflammation and cancer.
Analysis: The important shift is not merely image size. It is the ability to collect multiple physical parameters from the same cross-section. In principle, that broadens what clinicians might infer from ultrasound, especially where tissue stiffness, echogenicity, speed of sound, and attenuation change together.
Which applications did the researchers test?
Two applications stood out in the study. First, the system observed abdominal adipose distributions, allowing adipose thickness assessment without ionising radiation or mechanical deformation. Second, it demonstrated video-rate biopsy needle localization with respect to internal tissue features. In both cases, the clinical value comes from a wider view of anatomy combined with less distortion than traditional contact-based scanning.
Verified fact: The study frames these as unmet clinical needs currently not fully addressed by other modalities. The abdominal fat application is especially notable because it avoids radiation exposure and the tissue compression that can affect measurements. The biopsy localization application matters because it shows the system can support procedures, not just diagnosis.
Analysis: These are not abstract engineering demonstrations. They point to practical settings where a broader ultrasound field could improve measurement confidence and procedural guidance. The body of the evidence suggests the platform is being positioned as a clinical tool for situations where current methods either distort tissue, expose patients to radiation, or fail to capture the full cross-section.
Who benefits, and what remains unresolved?
Patients stand to benefit if the system can eventually be translated into routine care, especially where safe, repeatable, whole-cross-section imaging matters. Clinicians could benefit from less operator dependence and a larger field of view. The study also benefits a broader medical-engineering agenda at Caltech, because it presents ultrasound as a modality that can be expanded rather than simply refined.
At the same time, the available evidence is still bounded. The reported tests involved five healthy volunteers and focused on the abdomen and thighs. The study shows agreement with MRI counterparts, but it does not claim that the system is ready to replace MRI or other established tools. The reconstruction code is not publicly available because it is proprietary and may be used in licensed technologies. The full raw ultrasound datasets are also not publicly deposited because of size, though a representative dataset is available through institutional data-sharing arrangements.
Analysis: Those limits matter because they shape what can be independently verified and how quickly the method may spread. The technical achievement is clear; the path to clinical adoption is still narrower and less transparent than the headline result might suggest.
What should the public understand now?
The central question is not whether caltech has produced a clever imaging prototype. It has. The larger issue is whether the medical field is prepared to treat whole-cross-sectional ultrasound tomography as more than an experimental extension of a familiar tool. The study indicates that ultrasound can deliver whole-body cross-sections, transmission data, and procedural localization in one platform. It also shows that the technology’s long-standing limits were partly design choices, not just physical constraints.
That makes the next step less about celebration than scrutiny: how such systems are validated, what access rules govern the software and datasets, and how the method performs beyond early volunteer testing. If whole-cross-sectional imaging becomes clinically useful, the question will be whether health systems can adopt it in a way that is safe, transparent, and broadly usable. For now, caltech has shown that sound can reveal more of the body than the standard ultrasound model has allowed.





